Cervical cancer screening is one of the most effective ways to prevent cancer before it starts. If you have a cervix, you deserve clear guidance on what to expect, how often to test, and how results guide follow-up.
At our Mountain View clinic, our team provides compassionate, trauma‑informed care with options that respect your pace and preferences.
Pap Test vs. HPV Test: What Each Looks For
Pap test:
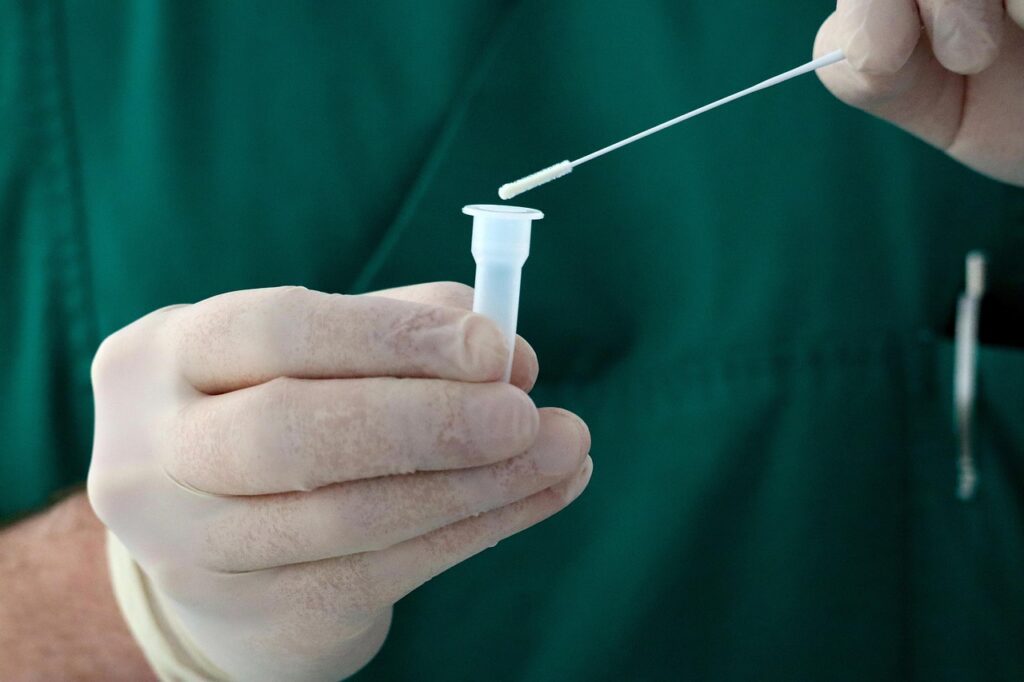
A clinician collects a small sample of cells from your cervix using a soft brush. A lab examines those cells for abnormal changes. The Pap does not test for the virus itself—it looks for precancerous or cancerous cell changes.
HPV test:
Uses a similar sample to detect high-risk human papillomavirus types that can cause cervical cancer. A positive HPV test does not mean you have cancer, but it may indicate closer follow-up is needed.
Both tests can be done at the same time during a pelvic exam. Collection typically takes less than a minute. You may feel pressure or brief cramping.
Current Screening Intervals by Age
These are common screening patterns for average-risk patients. Your schedule may vary based on history, results, and clinician guidance:
-
Under 21: No screening.
-
Ages 21 to 29: Pap test every 3 years.
-
Ages 30 to 65: One of the following, based on access and preference:
-
Primary HPV testing every 5 years, or
-
Co-testing with Pap and HPV every 5 years, or
-
Pap alone every 3 years if HPV testing is not available.
-
-
Over 65: Screening may stop if prior tests were negative and there is no history of high-grade changes. If there is a history of cervical precancer, continue screening for at least 20 years after treatment.
Special considerations:
If you are immunocompromised, had DES exposure, or prior high-grade abnormalities, you may need more frequent screening. Ask your clinician for a personalized plan.
How Results Guide Next Steps
-
Normal Pap and negative high-risk HPV: Continue routine screening on the recommended interval.
-
Normal Pap but positive high-risk HPV: Repeat testing in 1 year is common. Persistent HPV may prompt a colposcopy.
-
Abnormal Pap results (ASCUS, LSIL, HSIL): Management depends on age, HPV status, and risk. You may be advised to repeat testing sooner or have a colposcopy.
-
Colposcopy findings: Low-grade changes may be observed with close follow-up. High-grade changes are typically treated to remove or destroy abnormal tissue to prevent cancer.
Can You Request Cervical Cancer Screening?
Yes. You can request screening at any time, even if you are not due, especially if you have:
-
New symptoms
-
History of abnormal results
-
Known risk factors
Comfort and consent options:
-
Chaperones available
-
Female clinicians
-
Step-by-step consent
-
Smaller speculum options
-
Compatible lubricants
-
Option to pause or stop at any time
If an in-person visit is hard to schedule, start with a Palo Alto virtual gyn visit to plan next steps.
Common Questions We Hear Online
Do 90% of people have HPV?
Most sexually active people will get HPV at some point. Many clear the virus on their own within 1–2 years. Only a subset carry persistent high-risk types.
What is the #1 cause of cervical cancer?
Persistent infection with high-risk HPV, especially types 16 and 18. Vaccination, safer sex practices, and routine screening reduce this risk.
What is the first symptom of cervical cancer often?
Early cervical cancer usually has no symptoms. When symptoms appear, they may include abnormal vaginal bleeding, bleeding after sex, unusual discharge, or pelvic pain.
How late is too late for cervical cancer?
It is never too late to be evaluated. Screening is for people without symptoms. Symptomatic evaluation should happen immediately. Early detection improves outcomes at any stage.
Where does cervical cancer spread first?
It can grow locally in the cervix and nearby tissues such as the vagina, uterus, and pelvic lymph nodes before moving to distant sites. Screening aims to catch precancer before spread occurs.
Quick Myth Busters and Social Media Rules
-
The 2-week rule: See a clinician if symptoms like unexplained bleeding or persistent pelvic pain last more than two weeks. Don’t wait if you feel concerned.
-
Vaccination plus screening: Regular screening and HPV vaccination prevent the majority of cervical cancers over time.
-
HPV prevalence: Extremely common, but only persistent high-risk infections cause significant cervical changes.
When to Ask for Earlier Screening or Diagnostic Evaluation
-
New abnormal bleeding, including postcoital or between periods
-
Postmenopausal bleeding
-
Persistent pelvic pain or pressure
-
Unusual discharge, especially watery or blood-tinged
-
Prior abnormal Pap or positive high-risk HPV
-
Weakened immune system or new risk factors
If any of these apply, schedule an appointment promptly. Telehealth triage is available for urgent evaluation.
How Our Mountain View Clinic Supports You
You may want screening that feels private, unhurried, and centered on consent. At Renaissance Healthcare for Women, you can expect:
-
Calm visits
-
Stepwise explanations
-
Options tailored to your comfort
If you live nearby, we offer convenient access to cervical cancer screening in Palo Alto and gentle Palo Alto Pap smear services. We also coordinate mammograms, DEXA orders, contraception, and broader gynecologic care in one place.
Clinic location: Sobrato Pavilion, 2495 Hospital Drive, Suite 515, Mountain View, CA 94040
Call: (650) 988‑7830 to schedule or request a telehealth planning visit.
The Bottom Line
Pap and HPV tests work together to prevent cervical cancer. Start screening at 21, transition to HPV-based testing in your 30s, and follow your personalized interval.
Remember:
-
HPV is common
-
Early cervical cancer is usually silent
-
Persistent high-risk HPV causes most cases
If you are due or have symptoms, book your visit. We are here to make screening clear, comfortable, and timely.